Low Dose IL-2 and Rapamycin Leads to Prolongation of Human Islet Allograft Survival by Inhibition of IFN-gamma+ T cells and Expansion of FOXP3+CD25+ Tregs in a Humanized Islet Transplant Mouse Model
Min Hu1, Wayne Hawthorne1, Heather Burns1, Hai Nan1, Yi Wen Qian1, David Liuwantara 1, Elvira Jimenez Vera1, Yi Vee Chew1, Karen Keung1, Shounan YI1, Stephen I Alexander2, Philip O'Connell 1.
1Centre for Transplant and Renal Research, Westmead Institute for Medical Research, University of Sydney, Westmead, Australia; 2Centre for Kidney Research, Children's Hospital at Westmead, , Westmead, Australia
Introduction: We established a humanised mouse model with dominant human (h) CD3 T cells engraftment and showed it was capable of rejecting h-islet allografts. The study aims to develop a therapeutic regimen for expansion of Tregs and suppression of effector T cells to protect h-islet transplants (Tx) from rejection.
Methods: Strep-induced diabetic NOD/scidIL2rg-/- were transplanted with h-islets. After successful Tx, mice were reconstituted with1×107 h-spleen-cells and IL2 and/or Rapamycin (Rap) treatment. Protocols using IL2 and/or Rap included two doses of IL2 (0.3x106IU/1x106IU/m2) for 8 weeks (W), with/without Rap (0.5/1mg/kg) for 5 weeks (IL2 for 2W, IL2/Rap for 1W, IL2/Rap for 2W), and IL2/Rap for 3W.
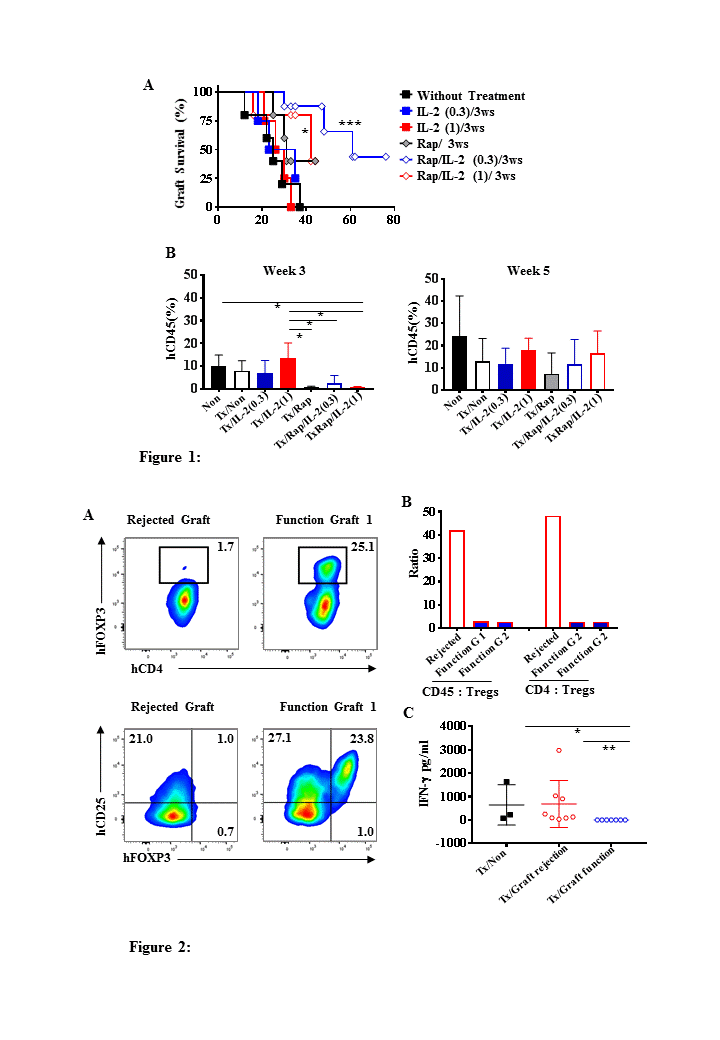
Results: The proportion of hFOXP3+ Tregs was reduced in humanized h-islet Tx recipients with rejection when compared with proportion of FOXP3+ Tregs found in the donor spleen (3.9%±1.6 at W5 vs 5.9% in donor’s spleen). This was similar to humanised mice without Tx (3.4%±1.0 at 5W & 0.9±0.5% at 9W). While there was no significant increase of hCD45+ cell engraftment in the two groups treated with IL2 treated for 8W (compared to no treatment group), an increase of proportion of Tregs occurred at 4W in IL2 1x106IU/m2 group, but it was unstable and loss of Tregs occurred at 9W (0.5±0.1%). Using this protocol T cells fully expressed CD25 which was not observed in other groups. For the 5W protocol, hCD45+ cell engraftment increased continually from 3W to 9W in the two IL2 only groups and the no treatment group. In the IL2/Rap groups the increase in hCD45+ engraftment plateaued after 7W. Meanwhile the proportion of hFOXP3+ T cells actually increased in the IL2/Rap groups at 9W (IL2(0.3)/Rap=15.8±5.0% and IL2(1)/Rap=22.6±17.7% p>0.05) when compared to controls the proportion of Tregs actually declined in the other groups [(0.9±0.5%, no treatment)(0.8±0.3%, IL2(0.3)(1.7±0.6%, IL2(1) at 9W). However these cells were FOXP3+CD25- cells, not FOXP3+CD25+ cells and GVHD still occurred in all these groups suggesting these cells were not regulatory rather effector T cells. However, the combination of low dose of IL2 with Rap for 3W led to significant prolongation of human islet allograft survival (MST of 61 days and 42 days in IL-2(0.3)/Rap (p <0.001) and IL-2(1)/Rap (p <0.05) respectively, whilst there was no prolongation of survival in animals treated with IL-2 alone (IL2(0.3) MST = 29 or IL-2(1) MST = 29 v no treatment MST=25) (Fig. 1A). There was a significant decrease in hCD45+ engraftment in mice treated with IL2/Rap and Rap at 3W (P<0.05) (Fig.1B) and the proportion of, hFOXP3+CD25+ Tregs was increased at 5W in IL2 with/without Rap Tx groups compared to non-Tx mice without treatment. In mice treated with IL-2(1)/Rap the proportion of CD25+FOXP3+ T cells was greater than that found in those mice who had rejected their grafts (Fig.2A). In addition the ratio of hCD45: hTregs was higher in the rejecting mice compared to mice with functional islet grafts at day 44 post reconstitution (Fig.2B). and a significant decrease in serum IFN-γ levels was observed in the humanised mice with functional grafts, when compared to mice with rejected grafts and no treatment (Fig.2C) .
Conclusions: IL-2/Rap treatment led to prolonged islet allograft survival, suppression of effector T cells in vivo and expansion of hFOXP3+CD25+ Tregs. Such a protocol may have clinical potential as a strategy to expand Tregs in the presence of antigen, in vivo, and could be used in conjunction with cell based therapy to prevent rejection.