Natural History and Determinants of Infectious Complications after Kidney Transplantation: A Nationwide Prospective Population Based Cohort
Anne Scemla1, MC Perrier1, Olivier Lortholary1, S Girerd1, C Kerleau1, V Garrigues1, F Burron1, N Kamar1, C Legendre1, Yassine Bouatou1, C Lefaucheur1, M Giral1, Alexandre Loupy1.
1Paris Transplant Group, INSERM, Paris, France
Background: Although infectious complications are recognized as a major cause of morbidity and mortality in kidney transplant recipients (KTR), little is known about their natural history and determinants at a population level.
Methods: Nationwide cohort including all consecutive KTR from 6 French centers (2000-2012) with prospective uniform, and quality-checked collection of baseline characteristics, events during follow-up, together with a systematic record of post-transplant infections (e.g. site and pathogen).
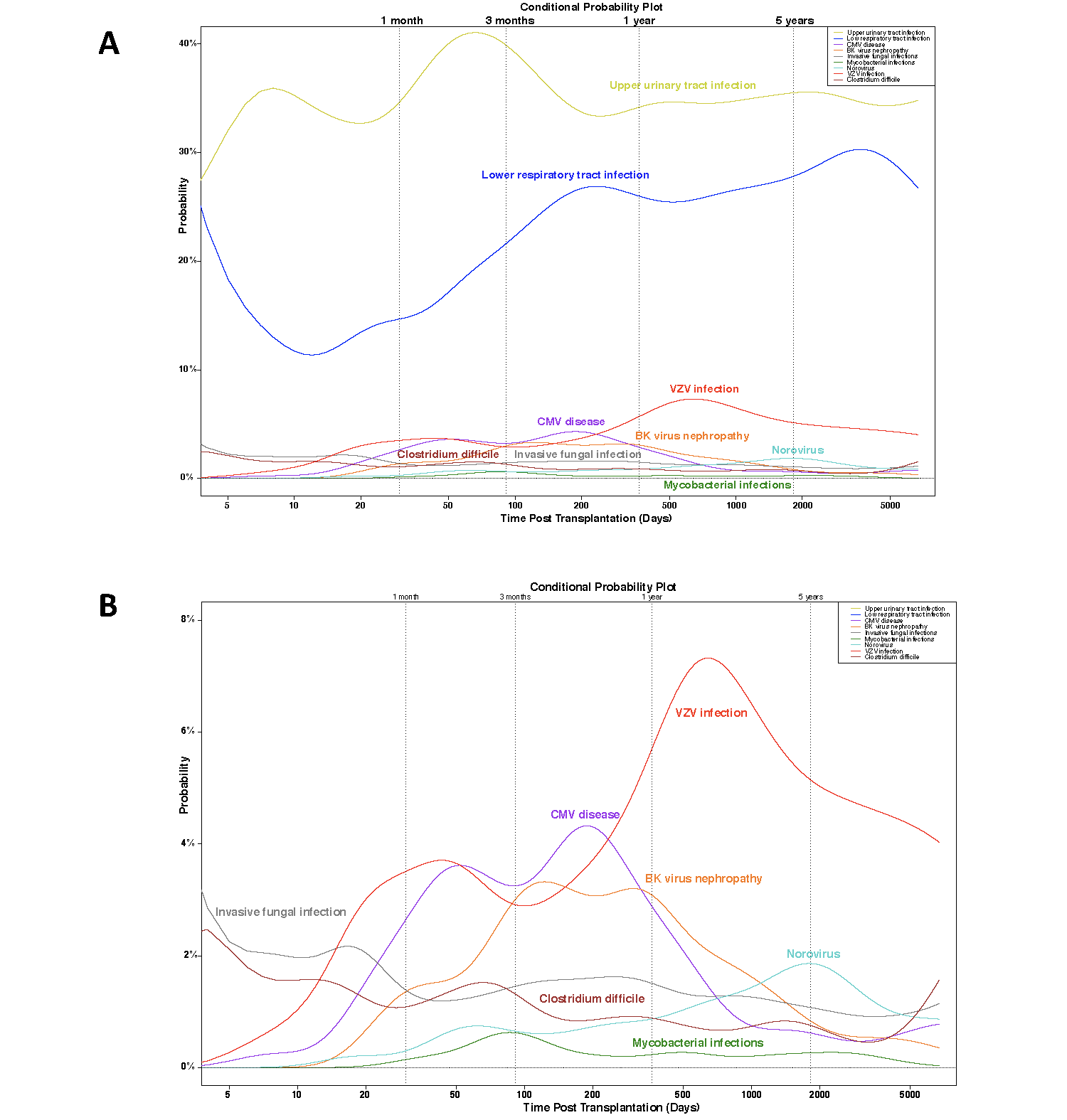
Results: 8,398 KTR were included with a median follow-up post-transplant of 7 years (IQR 4-10; 56,916 patients-years). During the follow-up, 11,014 infections were diagnosed in 4,695 patients. The first episode occurred after a median 177days (IQR 20 – 939) after KT. Infections were bacterial (n=9,123, 82.8%), viral (n=1,546, 14 %), fungal (n=297, 2.7%) or parasitic (48, 0.4%). Main sites were upper urinary tract (n=4,232, 38.4%), lower respiratory tract (2,703, 24.5%), blood stream (n=908, 8.2%), skin (750, 6.8%), and GI tract (n=616, 5.6%). Main pathogens identified during infections were Enterobacteriaceae (3,094, 28.1%), Staphylococcus sp (771, 7%), VZV (496, 4.5%), Enterococcus sp (482, 4.4%), Pseudomonas sp (386, 3.5%), CMV (209, 1.9%), BK virus (191, 1.7%), HSV (156, 1.4%), norovirus (111, 1%); P. jiroveci (96, 0.9%), Candida sp. (94, 0.9%), and Aspergillus sp. (85, 0.8%). The conditional probability of infection occurrence over time is in Figure 1. Infection was associated with an increased risk of death (p<0.001). The independent determinants of time to infection were: recipient age, female gender, diabetes, hypertension, major cardiovascular events, induction treatment, eGFR at 1-year post KT, acute rejection, donor age and graft rank (p<0.001 for all comparisons).
Conclusion: In this first systematic population-based assessment of infections after KT, we show the potential for a data driven approach with post-transplant infectious trajectory prototypes that would help clinicians improve the clinical management through patient risk stratification for immunosuppressive regimens adaptation.