Circulating Follicular Helper T Cells (cTfh) in Renal Transplantation: Utility as Rejection Biomarker
Rocio Laguna Goya1, Alberto Utrero Rico1, Francisco Cano Romero1, Elena Gomez Massa1, Daniel Arroyo1, Pilar Auñón Rubio2, AM Sevillano Prieto2, Maria José Castro Panete1, Amado de Andrés Belmonte2, Estela Paz Artal1.
1Immunology, Hospital 12 de Octubre, Madrid, Spain; 2Nephrology, Hospital 12 de Octubre, Madrid, Spain
Introduction: Antibody mediated rejection is responsible for 30-50% of renal graft failures. Follicular helper T cells (Tfh) are required for the differentiation of B cells into plasma cells and for the efficient production of antibodies. Recently, circulating follicular helper T cells (cTfh) have been identified in peripheral blood; this facilitates the study of cTfh as potential biomarker in renal transplantation. With this background, the aims of our study are: (1) to show the capacity of cTfh to differentiate B cells into plasma cells and produce antibodies, (2) to study cTfh in chronic kidney disease patients pretransplantation, (3) to follow up variations in cTfh posttransplantation and (4) to correlate differences in cTfh distribution with graft outcome.
Methods: We isolated peripheral blood mononuclear cells at pre-transplantation and at 7 and 14 days and 1, 3, 6 and 12 months post-transplantation from a prospective cohort of renal transplantation recipients (n=163). We analyzed cTfh by flow cytometry as CD4+CXCR5+ or CD4+CXCR5+CCR7lowPD1high. cTfh were cocultured with B cells to interrogate their capacity to stimulate conversion to plasmablasts and antibody production. Clinical and immunological data were prospectively collected.
Results: First, we showed that when co-cultured with cTfh, B cells differentiated into plasmablasts and produce IgG.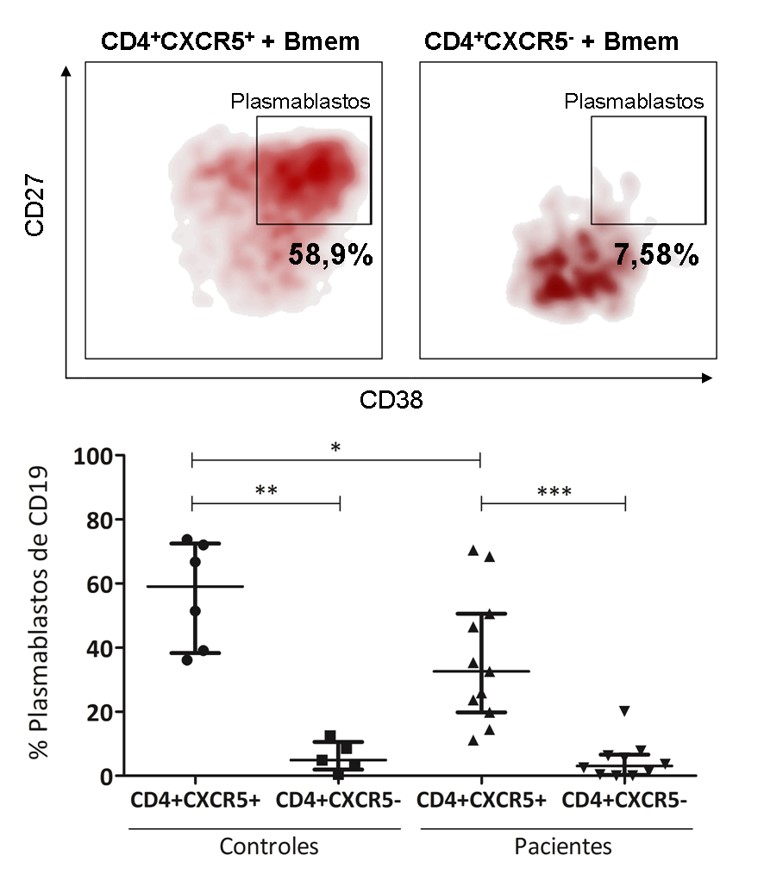 Pretransplantation, cTfh were decreased in patients who had received dialysis compared to those directly transplanted (p<0.01). Conversely, cTfh were increased in retransplanted patients, in those with previous blood transfusions and in patients with anti-HLA antibodies pretransplantation (sensitized patients) (p<0.05, all comparisons). During follow-up, cTfh decreased a week after transplantation in patients who received thymoglobulin as induction therapy (p<0.05) and started to increase three months after transplantation. Patients who received thymoglobulin tripled their cTfh six months posttransplantation. Basiliximab treatment did not deplete cTfh. We explored the utility of cTfh as biomarker in renal transplantation and found that cTfh were increased pretransplantation in patients who will develop de novo anti-HLA antibodies and in patients who will have a rejection compared to patients who will not do so (p<0.05, both).
Pretransplantation, cTfh were decreased in patients who had received dialysis compared to those directly transplanted (p<0.01). Conversely, cTfh were increased in retransplanted patients, in those with previous blood transfusions and in patients with anti-HLA antibodies pretransplantation (sensitized patients) (p<0.05, all comparisons). During follow-up, cTfh decreased a week after transplantation in patients who received thymoglobulin as induction therapy (p<0.05) and started to increase three months after transplantation. Patients who received thymoglobulin tripled their cTfh six months posttransplantation. Basiliximab treatment did not deplete cTfh. We explored the utility of cTfh as biomarker in renal transplantation and found that cTfh were increased pretransplantation in patients who will develop de novo anti-HLA antibodies and in patients who will have a rejection compared to patients who will not do so (p<0.05, both).
Conclusions: There are differences in cTfh between patients with different characteristics, mainly related to HLA sensitization. Pretansplantation cTfh measurement could be a useful non-invasive biomarker, enabling us to predict renal graft outcome and, therefore, to take early preventive measures to avoid graft failure.
Fundación de la Sociedad Madrileña de Trasplante (Expediente I+12: 2017/082). Instituto de Salud Carlos III (PIE13/00045).
