
Hospital Course after TAH Implantation, Nebraska Experience
Heather Chambers1, Andre Kalil1, Diana F Florescu1.
1Transplant Infectious Diseases, University of Nebraska Medical Center, Omaha, NE, United States
Background: Total artificial heart (TAH) implantation has become a reliable bridge to heart transplantation. This study looked at the hospital course, including infectious complications, after TAH-t.
Methods: This is a retrospective study of adult patients who underwent a TAH-t at our institution from 2013 through 2017. All continuous variables were reported as medians and respective ranges. All categorical variables were analyzed as proportions. Kaplan-Meier survival analysis was used to assess time-to-infection, time-to-transplant, and time-to-death.
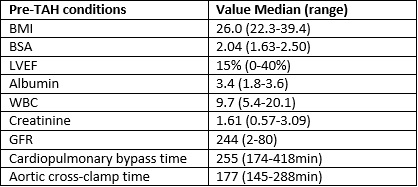
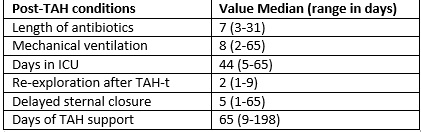
Results: Nine patients were included in the study with median age of 48 years (21-61 years); 78% (7/9) were male. Table 1 presents patients’ characteristics prior to TAH-t. 33% (3/9) of patients had a previous IABP, 22% (1/9) a prior heart transplant, 22% (1/9) ECMO, and 11% (1/9) had a LVAD. 22% (1/9) of the patients had baseline diabetes and 56% (5/9) chronic renal failure. 11% (1/9) of the patients required renal hemofiltration after TAH-t. 67% (7/9) of patients had delayed sternal closure with one patient expiring 65 days post-op with sternum still open. 78% of patients had at least one infection. The most common infections were bloodstream infections (5 patients) followed by pneumonia (4 patients), diagnosed at a median of 58 days (16-127 days) and 102 days (11-125 days) after TAH-t.
The median time from TAH-t to the first infection was 15 days (5-32 days) and from the TAH implantation-to-death 2 months (0-16 months); the median time-to-transplantation was 3.5 months (2-6 months).
Conclusion: Patients are critically ill prior to TAH-t and required prolonged support in the ICU and multiple interventions after surgery. Infections are common in patients who receive a TAH with the most common infections being bloodstream infections and pneumonia.
