Comparison of Sleep Quality in Hemodialysis Vs Kidney Transplant Recipients using Pittsburgh Sleep Quality Index (PSQI)
Shafiq Ahmad SAC Chughtai 1, Beenish BA Afzal 1, Jean JS Scott 1, Shakeeb SK Khan 1, Rajagopal RP Poyyamazhi 1, Mayer MGA Ghazal Aswad 1, James JY Yates 1, John JB Black 1, Anna AR Rizello1, Ahmed AA Ali 1, Tahir TD Doughman 1, Atul AB Bagul 1.
1Leicester General Hospital , University Hospital of Leicester , Leicester , United Kingdom
Background: Disturbed sleep causes depression and poor health related quality of life (HRQoL). Studies have shown that poor sleep quality is an independent predictor of mortality in patients with end stage renal disease (ESRD). To compare the effect of kidney transplantation (KT) on sleep quality, we did a prospective study comparing patients on haemodialysis (HD) with kidney transplant recipients.
Material and Methods: Pittsburgh sleep quality index (PSQI) was used to assess 40 patients each following KT and those undergoing HD. A PSQI score of 5 or more was considered indicative of poor sleep quality. All patients were requested to fill the questionnaire (self-assessment) while attending for HD sessions or follow up clinics. All transplant recipients were within 6 months of kidney transplantation and were not dependent on HD at the time of filling the questionnaire.
Results: There were 40 respondents in each group. Mean age in KT group was 50.7 years (21-75 years, 62% Males, 38% Females). In HD group mean age was 62.3 years (26-90 years,64% Male and 36% Females). Those with previous psychiatric history were excluded. In KT group, 15 out of 40 (37.5%) had PSQI score of more than 5 (poor sleep). In HD group, 32 out of 40 (80%) had PSQI score of > 5 and thus poor sleep (p< 0.5). The highest PSQI score was 17 in KT and 16 in HD group.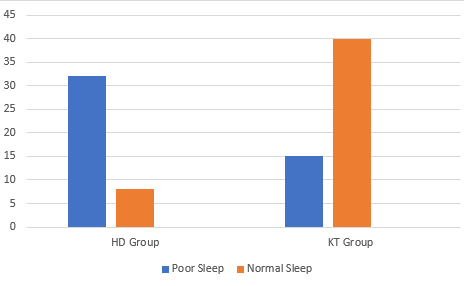
Pain was one of the biggest reasons in both groups for sleep disturbance. Most of the respondents reported better sleep quality prior to the development of kidney disease. Reasons for poor sleep are multifactorial and include medications, increasing age, chronic ill health and presence of co morbidities however both of these groups were relatively age matched and had same subsets of co morbidities.
Conclusion: Incidence of poor sleep was much higher in patients on HD when compared with KT recipients. Hence, we can conclude KT improved sleep quality. Even after transplantation, the proportion of respondents reporting sleep disturbances was higher than general population. Poor sleep quality continues to adversely affect HRQoL. Further research and clinical attention for sleep disturbances in these patients is warranted.
